Joint Replacement
Considering Hip or Knee Joint Replacement?
Hip and knee arthritis can cause a significant amount of pain, which can seriously limit your quality of life. Replacing the joint offers relief from that pain, helping you to get back to the lifestyle you enjoy. Dr. Davis desires to help every patient regain their quality of life and get back to an active lifestyle. He uses an individualized patient-centered approach and the most up-to-date techniques.

What Is Hip Arthritis?
Hip arthritis is caused when the smooth cartilage found in the hip joints wears out. Normally the cartilage in a hip joint allows for free motion and painless walking. In hip arthritis some or all of that cartilage is lost, creating rough surfaces. Bone starts to rub on bone, causing pain and inflammation.
What Is Knee Arthritis?
Knee arthritis, like other arthritis throughout the body, is simply when the nice, smooth cartilage we normally have in our joints wears out. In healthy bones, this cartilage allows for smooth movement as you walk or move. If the cartilage in your knee joint wears out, the bone surfaces that rub together become rough. This can cause pain and swelling and may also limit your range of motion.


What Non-surgical Options Are Available?
Prior to any surgery, you can try treating hip or knee arthritis with medication, such as Tylenol or anti-inflammatories like ibuprofen. Cortisone or joint injections can also help to decrease swelling and relieve pain. Before undergoing a replacement, some patients benefit from non-surgical options like these:
- Medication, including Tylenol or anti-inflammatories like ibuprofen
- Cortisone injections
- Gel or synthetic injections
- Platelet-rich plasma (PRP) or stem cell injections
What Joint Replacement Is Right for Me?
"Each patient has a different experience as they go through life and have to deal with their joint pain, so I really focus on individualized care. During your first visit I’ll typically start with a conversation to learn about your history and how joint pain is affecting your quality of life. Next, I’ll do an examination to see what limitations you may have around your hip or knee. We’ll also get some X-rays to determine the extent of any arthritis you may have, which I’ll review with you to help you understand exactly what’s causing your pain or other concerns. If surgery is an option, we’ll have a full discussion about the process, including the typical schedule, what your recovery will look like, what you can expect going forward, and answer any other questions you may have."
Dr. Davis
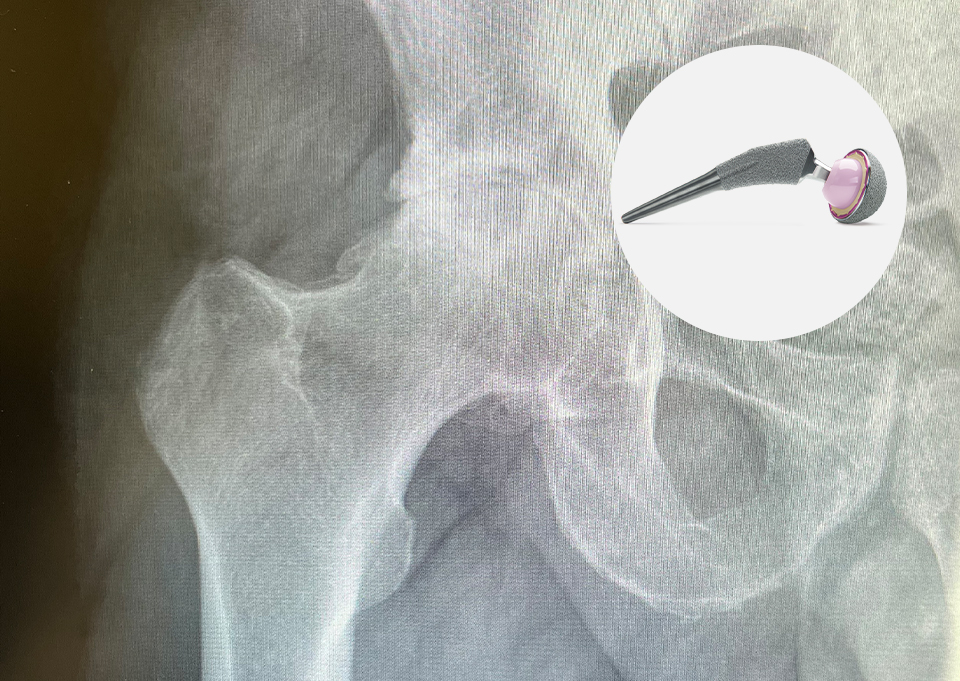
What Is a Hip Replacement, and How Does It Relieve Pain?
A hip replacement can be performed through an incision directly in the front of your thigh or along the side. Either way the end result is the same. Damaged bone and cartilage are removed, a new cup is placed inside of your pelvic bone, and a plastic or polyethylene liner is locked inside of it. In addition, a metal stem with a ceramic head is fitted to the top of your thigh bone. When you walk or move your hip after surgery, your new hip replacement moves smoothly, eliminating the rubbing of rough bone that caused the pain and inflammation.
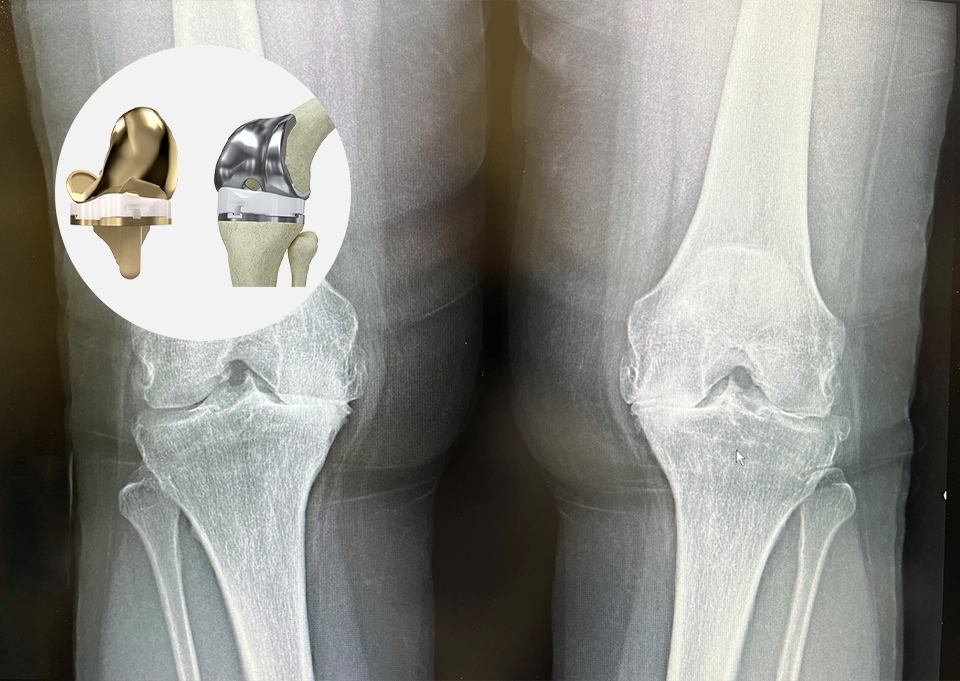
What Is a Total Knee Replacement, and How Does It Relieve Pain?
Total knee replacement is simply a resurfacing of the end of your bone and your knee joint, which includes the femur (your thigh or upper leg bone) and the tibia (the larger bone in your lower leg). To perform the procedure, we make an incision directly down the center of the knee, remove the bad cartilage on the end of the femur and replace it with a metal cap. We also cement a metal tray at the top of your tibia, along with a plastic piece that locks in between. Your kneecap is then resurfaced with a plastic “button” on the underside of the bone. So, when you walk or bend your knee after the surgery, the joint moves smoothly again — it’s all metal-on-plastic parts. This relieves your pain because there are no nerve endings within the knee replacement. Nowadays, a knee replacement should last you 20 to 30 years.
What Is a Partial Knee Replacement, and How Does It Relieve Pain?
In a select group of patients with arthritis a partial knee replacement may be your best option. Partial knee replacement is a resurfacing of the end of your bone as with a total knee replacement. The difference is we only resurface the part of the knee that is affected by the arthritis (most commonly the medial or inner part of the knee). To perform the procedure, we make a smaller incision on the front of the knee, remove the bad cartilage on the end of the femur and replace it with a metal cap. We also cement a metal tray at the top of your tibia along with a plastic piece in between. So, when you walk or bend your knee after the surgery the joint moves smoothly again. With a partial knee replacement your normal ACL and PCL ligaments remain intact, so the knee can feel more natural than a total knee replacement. A pain-free knee is always the goal! A partial knee replacement should last 20 to 30 years.

Surgery Day & Recovery
Can I go home the same day of surgery?
YES! Outpatient hip and knee replacement is becoming more and more common. Gone are the days where you spend multiple days in the hospital.
“I encourage almost all of my patients to go home the same day of surgery. Whether you are having a first-time hip or knee replacement, or even a revision (or reoperation) surgery, our team will work hard to get you home!” Dr. Davis
What does my surgery day look like?
When you arrive the morning of surgery, you will be evaluated and prepared for surgery by our trained nursing staff. The anesthesia team will then talk with you about your options, including a spinal anesthesia, which lessens the number of medications you will need, allows you to wake up faster, and also decreases your pain after surgery. Dr. Davis will then come talk with you, answer any additional questions you have, and offer to pray with you.
After the surgery is complete and you have woken up, you will go to the outpatient recovery room. You will get something to eat and drink and our mid-level provider (nurse practitioner or physician assistant) will talk with you, write your prescriptions, and go over specific discharge instructions. Our physical therapy team will then help you walk for the first time with your new joint replacement! You can even walk up and down stairs if you have them at home.
We ensure that you and your support team are comfortable with all aspects of going home. We even get your first outpatient physical therapy appointment arranged before you leave.
After that, HOME it is! Our goal is to make the transition from surgery to home as smooth as possible.
What about physical therapy?
“With the help and encouragement of a physical therapist, I see my patients recover at a quicker pace and get back to enjoying life without limitations.” Dr. Davis
Physical therapy plays a very important role in your recovery after joint replacement. This will start on the day of surgery where you will meet and work with our talented physical therapy staff. They will help you get up for the first time, walk the halls and even walk stairs if you have them at home. Within a day or two of leaving the hospital or surgery center, you will have an appointment to work with an outpatient physical therapist. Depending on the surgery (hip or knee) you will work 1-3 times a week with them for about 6 weeks.
After surgery, your job and the role of the therapist, is to decrease swelling around the surgery site, regain your joint range of motion, and continue to strengthen the muscles supporting your new joint replacement.

